Food list – What to eat and avoid. The 1. 7 Day Diet (2. Start with high lean protein, high non- starchy vegetables, probiotics, no starches. Add unprocessed starch foods and slowly increase the allowed amount of fat in animal protein foods. Add other whole grain starches and more ingredient choices. Maintenance diet.
No sugars, bad fats (saturated, trans), low salt. Below. Send this page to friends, family, and anyone else who you want to understand what you. Mike says “This book is my attempt over the last two years to fix and tweak the original 1. Day Diet so that you can lose weight even faster, keep it off longer, and stay healthy and fit well into your golden years.”Also get a copy of The 1. Day Diet Cookbook for more recipes.

The reasoning behind The 1. Day Diet. This diet claims to use . By avoiding processed foods, sugars, and bad fats, you can improve your health and lose weight. The diet has 4 cycles. Cycle 1: Accelerate. This cycle claims to promote rapid weight loss by improving digestive health, helping clear sugar from the blood to boost fat- burning, and discourage fat storage. You follow this cycle for 1.
- Managing an appropriate diet for an EPI dog is extremely important but can be the most confusing aspect to managing EPI since finding the "best" diet really depends.
- The Fast Metabolism Diet by Haylie Pomroy (2013): What to eat and foods to avoid.
- For everyone who asked for a simplified, essentials-only version of the diet I advocate in Wheat Belly, here it is. This is the very same diet I advise for patients.
If you reach your weight loss goal you move to cycle 4; if not you move to cycle 2. This cycle can also be used if you gain some weight back and want to quickly lose it. Cycle 2: Activate. This cycle claims to reset your metabolism through a strategy that involves increasing and decreasing your caloric consumption to stimulate fat- burning and to help prevent plateaus. It lasts 1. 7 days and consists of alternating between Accelerate days (see above) and Activate days, where you start to add natural starches. Cycle 3: Achieve.
This cycle claims to help you develop good eating habits through the re- introduction of additional foods and move you closer to your weight goal. Some more carbs are allowed, and protein is cut down.
At the end of cycle 3, if you have additional weight to lose, you can recycle back to cycle 1 then 2 then 3, or 2 then 3, or continue with 3 until you reach your goal weight. Cycle 4: Arrive. This cycle claims to keep you at your goal weight through a program of eating that lets you enjoy your favorite foods on weekends, while eating healthfully through the week. Monday breakfast through Friday lunch, eat with restrictions as described in cycles 1, 2, or 3. Friday dinner through Saturday night, eat your favorite foods and meals in moderation. There are some foods that you should always avoid on this diet, plus different foods to eat and avoid on each phase/cycle. In the Breakthrough Edition, there’s an optional Transitional Day Fast between cycles.
There are also guidelines to follow if you have PMSThe author says that this diet is designed for people in normal health – you should not follow this diet if you have type 1 diabetes, any serious medical disease, or if you are pregnant or breastfeeding/nursing. Always avoid these foods. Mike suggests in the Breakthrough Edition. He says it can help reduce cardiovascular disease, blood pressure, gastrointestinal troubles, type 2 diabetes, cholesterol levels, and chronic inflammation, as well as increasing fat- burning and sparing lean muscle.

He also says it will accelerate your results. Drink 3 Fat- Burn Smoothies throughout the day: one at breakfast, one at lunch, and one at dinner.
Ingredients are whey protein powder, unsweetened almond milk, and other ingredients such as low- fat yogurt, powdered fiber, crushed pineapple, banana, strawberries, fresh spinach, matcha green tea powder, and Truvia. Day Diet cycle 1 – food list. Cycle 1. These are marked here with a *star. Cycle 1 contour foods are fish, apples and pears, olive oil, and yogurt.
Lean proteins . Opt for wild- caught rather than farm- raised fish. Poultry: skinless chicken breasts, skinless turkey breasts, lean ground turkey.
These lean proteins are also listed as acceptable in cycle 1 in the ethnic diets section of the book: ceviche; red snapper (huachinango)Eggs . Stick to no more than 4 yolks per week if your physician has diagnosed you with high cholesterol. Egg whites can be eaten without restriction in the original diet; the Breakthrough Edition says that 4 egg whites = 1 serving. Cleansing vegetables .


Plenty to choose from. Whether following a low carb diet, or wanting to find a snack that has little effect on blood sugar levels, there Eating a healthy low-fat diet is much easier when you have a list of low-fat foods as a resource. Low-fat diets give increased protection against the risk of heart.
Do not eat fruit after 2pm*Apples, berries (all types), grapefruit, oranges, peaches, *pears, plums, prickly pear cactus, prunes, red grapes. If you take statins and want to eat grapefruit – have. Consult with your physician before doing this.
Fruits and vegetables should be eaten raw whenever possible, except carrots and tomatoes. Greek- style, sugar- free fruit flavored, plain, low- fat . So the first day of cycle 2 you eat the foods listed below, the second day you eat the foods listed in phase 1 only, and so on alternating between the two. Cycle 2 Activate days: .


These are marked here with a *star. Do not eat natural starches after 2pm*Whole grains (1 serving = . On the alternate Active days, avoid the . These are marked here with a *star. Do not eat fruit after 2pm. Apricots, *bananas, cherries, currants, figs, kiwi, kumquats, guava, mango, papaya, pineapple, pomegranate, tangerine, tangelo, virtually any fresh fruit. Probiotics, dairy, and dairy substitutes: 1- 2 servings daily.
Low- calorie cheeses (brie, camembert, fontina, low- fat cheddar, edam, feta, goat, limburger, part- skim mozzarella . Eat slowly and enjoy your food. If desired, enjoy alcoholic drinks in moderation over the weekend (1- 2 daily) . Eat your heaviest meal around noon. Health benefits claimed in The 1. Day Diet. This diet claims to reduce the risk of cancer. Consult your doctor before starting a new diet.
This page describes what the authors of the diet recommend – Chewfo is describing the diet only, and does not endorse it. See the original 1. Day Diet for more information on the foods that are encouraged at each stage, the benefits of friendly gut bacteria, why to drink a lot of water, the exercise plans.
Health Benefits of Fiber You May Not Know. By Dr. Mercola. Public health guidelines from the US Food and Drug Administration (FDA) advise Americans to eat between 2. This isn't surprising, since fiber refers to the indigestible portion of plant foods, and in the largely refined standard American diet, healthful fibers are often processed right out. Unless you regularly eat whole fruits and vegetables, nuts, and seeds, you may be missing out on the healthiest forms of fiber available – and that could be a problem. That said, in spite of their fiber content, bulking up your diet with bran muffins and cereal is typically a big mistake, which I'll explain shortly. Why Is Fiber So Important? I've long been interested in the health benefits of fiber.
In fact, when I was in medical school 3. I was so convinced of fiber's many benefits that my nickname was Dr. I've since come to appreciate that the type of fiber in your diet, as well as your gut health, play a major role in harnessing fiber's health potential while avoiding its potential pitfalls.
Before I explain, let's go over a bit of fiber basics. Soluble fiber, like that found in cucumbers, blueberries, beans, and nuts, dissolves into a gel- like texture, helping to slow down your digestion.
This helps you to feel full longer and is one reason why fiber may help with weight control. Insoluble fiber, found in foods like dark green leafy vegetables, green beans, celery, and carrots, does not dissolve at all and helps add bulk to your stool.
This helps food to move through your digestive tract more quickly for healthy elimination. Many whole foods, especially fruits and vegetables, naturally contain both soluble and insoluble fiber. Health Benefits of Fiber.
There's no shortage of research showing how fiber may boost your health. Some of its top potential benefits include: Blood sugar control: Soluble fiber may help to slow your body's breakdown of carbohydrates and the absorption of sugar, helping with blood sugar control.
Heart health: An inverse association has been found between fiber intake and heart attack, and research shows that those eating a high- fiber diet have a 4. Stroke: Researchers have found that for every seven- grams more fiber you consume on a daily basis, your stroke risk is decreased by 7 percent. Weight loss and management: Fiber supplements have been shown to enhance weight loss among obese people,3 likely because fiber increases feelings of fullness. Skin health: Fiber, particularly psyllium husk, may help move yeast and fungus out of your body, preventing them from being excreted through your skin where they could trigger acne or rashes.
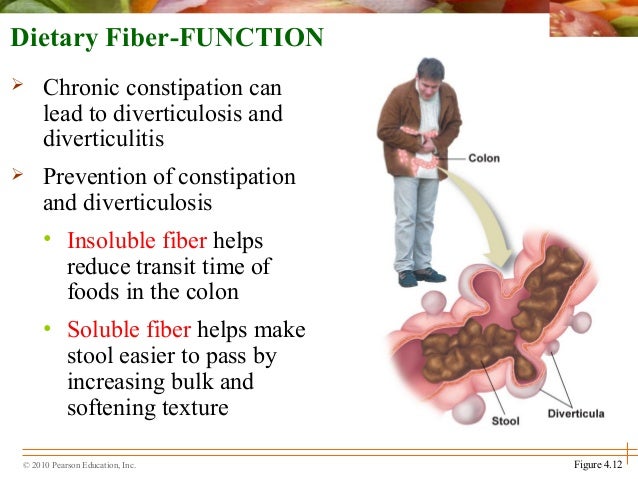
Diverticulitis: Dietary fiber (especially insoluble) may reduce your risk of diverticulitis – an inflammation of polyps in your intestine – by 4. Hemorrhoids: A high- fiber diet may lower your risk of hemorrhoids. Irritable bowel syndrome (IBS): Fiber may provide some relief from IBS. Gallstones and kidney stones: A high- fiber diet may reduce the risk of gallstones and kidney stones, likely because of its ability to help regulate blood sugar.
Wait: Read This Before You Stock Up on Bran Muffins! Loren Cordain, a professor at Colorado State University and an expert on Paleolithic lifestyles, humans are NOT designed to eat grains, and doing so may actually be damaging to your gut. Dr. That's the problem with the USDA recommendations. They think we're hardwired as a species to eat grains. You can get by just fine and meet every single nutrient requirement that humans have without eating grains. And grains are absolutely poor sources of vitamins and minerals compared to fruits and vegetables and meat and fish.
Ironically, since we're often told that whole grains are one of the best sources of fiber for our health, the high- fiber bran portion of grain – a key part that makes it a whole grain - - actually contains many of the anti- nutrients. Leaky gut can cause digestive symptoms such as bloating, gas, and abdominal cramps, as well as cause or contribute to many others symptoms such as fatigue, skin rashes, joint pain, allergies, psychological symptoms, autism, and more. All grains contain glutinous proteins known as prolamines that can be very . Plus, while fiber may be good for blood sugar, grains are not and may worsen health conditions like diabetes. Further, if you eat a high- fiber diet with a damaged gut, it can lead to serious problems. If Your Gut Isn't Healthy, a Temporary Very- Low- Fiber Diet May Help.
If you have chronic digestive symptoms like diarrhea, flatulence, stomach pains, reflux, leaky gut syndrome, food allergies, or intolerance, you'd be wise to implement the GAPS program. GAPS stands for Gut and Psychology Syndrome.
It also stands for Gut and Physiology Syndrome. The first part of the GAPS Introduction Diet is to remove fiber because it feeds microbes. The human digestive system is not designed to break down fiber. Instead, it ends up undigested in your bowel, where the majority of your gut flora resides. If your gut flora is healthy, i. However, if your gut is filled with pathogenic bacteria and/or yeast and fungi, fiber will actually make your symptoms worse, as it is a non- specific growth factor for intestinal bacteria, and does not discriminate between pathogenic and beneficial bacteria.
The digestive system of those with GAPS is predominantly populated by pathogens, which is why fiber must be carefully eliminated from your diet, for a period of time, to help starve out the pathogens (probiotic- rich fermented vegetables and soups with well- cooked, deseeded and peeled vegetables, such as zucchinis and squash, are allowed in the introductory phase). If you're interested in trying this out, I highly recommend getting Dr. Natasha Campbell- Mc. Bride's book Gut and Psychology Syndrome, which provides all the necessary details for the protocol. What Are the Healthiest Sources of Fiber?
Assuming your gut is generally healthy, I believe most people need upwards of 5. Most Americans get nowhere near this amount.
As the New York Times reported: 7. Instead, focus on eating more vegetables, nuts, and seeds. The following whole foods, for example, contain high levels of soluble and insoluble fiber. Chia seeds. Vegetables such as broccoli and Brussels sprouts.
Root vegetables and tubers, including onions and sweet potatoes. Psyllium seed husk, flax, and chia seeds.
This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Clients provided informed consent to veterinarians to prescribe PEPPS to 3. A 2 day/4 dose response rate, determined by veterinarians’ consensus, provided clinical threshold for a significant clinical outcome. Data was collected through phone interviews conducted over a period of 3. June 2. 00. 3 through December 2. PEPPS within 2 days or four doses. PEPPS within 2 days or four doses.
PEPPS appears useful for managing vomiting and diarrhea in dogs and cats. However, a randomized blinded placebo controlled trial is needed to quantify true clinical efficacy. Introduction. Timely management of disruptive gastrointestinal (GI) symptoms poses a challenge to both veterinary and medical physcians alike . Restoration of normal GI function requires effective means to mitigate nausea, vomiting, diarrhea, in dogs and cats .
Current approaches in managing nausea (usually observed as inappetence), vomiting and diarrhea in small animals involve supportive care, bowel rest, pancreatic enzyme supplementation and/or appropriate anti- microbials . Management of mucosal erosions and ulceration in small companion animals centers on control of acidity, either by neutralization with antacids, reduction with histamine- 2 blockers (e. A simplified approach in managing disparate GI symptoms would be useful for clinical veterinary practice were it safe, efficient and minimally burdensome . According to American Medical Veterinary Association . This translates into 1. Appendix A) that involve diagnostic workups and treatment plans for vomiting and diarrhea. This volume however only reflects the owners who actively utilize veterinarian services.
A recent survey of dog and cat owners . The survey implies that the estimated number of annual visits represents an undersized minority of animals that are actually affected. Given such a pervasive problem, any therapeutic intervention that improves management of disruptive GI symptoms would be a positive development.
Veterinary use of phyto- mucilages, particularly slippery elm, for gastrointestinal have been suggested by some . A potency- enhanced version of elm USP, requiring less than 1. Veterinarians were familiar with the 2. Gastrafate. Following successful preliminary testing . This report presents observational data from the use of polyanionic phyto- saccharide of elm mucilage (PEPPS) in practice- based settings of small animal veterinarians.
Potency Enhanced Polyanionic Phyto- Sac Charide. Elm mucilage USP is a polyanionic phyto- saccharide . Unlike sucralfate, PEPPS contains no aluminum or sulfate. Chiefly a high molecular weight mucilage (> 2.
Daltons), it is comprised of galactose- rhamnose disaccharides. Potency- enhanced elm phyto- saccharide is prepared by suspending elm mucilage in an anion- cation solution similar to that used to formulate high potency sucralfate (HPS) . The resultant potency- enhanced phyto- saccharide (PEPPS) is muco- specific and capable of attaining augmented surface concentration of slippery elm. With sucralfate, potency enhancement ranges from 7 - 2.
GI lining and higher fold increase on inflamed or injured mucosa. The exact postadministration surface concentration of PEPPS is unknown.
However, with PEPPS the concentration of elm USP administered is less than 8% the slippery elm dose recommended by holistic veterinarians . The formulation strength of Elm USP in PEPPS for small animals is 0. Administration of PEPPS was in accordance to weight. On average dogs or cats weighing less than 2. Dosing Administration. Participating veterinarians prescribed PEPPS in accordance to weight- dose chart in label instructions. PEPPS was given twice daily with food for the majority of the patients.
In the cases where vomiting and diarrhea disrupted eating and require intravenous hydration, PEPPS was given orally without food. Study Design—Observational Trial. This study was an open labeled non- blinded observational trial.
Information was collected regarding (a) weight of the dog or cat and (b) the nature and length of their GI symptoms at time of adding PEPPS. The length of illness is not reported. As an observational study, treatment intervention was not randomized.
By design, differences in outcomes are observed without regard to similarities or dissimilarities of patient characteristics prior to treatment. In fact, in this type of study, treatment decisions were made by veterinarians prior to use of PEPPS, the selection of PEPPS being made by the veterinarian due to concern that pre. PEPPS treatments were ineffectual. In this trial the question addressed is not one of the efficacy of PEPPS. Instead the question addressed is one of the relative merits of PEPPS as a competing treatment or intervention.
Outcome of merit is relative to the expectation of the participating veterinarians. As discussed below a clinical response of 2 days or 4 doses merited note to the veterinarians involved. This study reports the percentage of dogs and cats with vomiting and diarrhea who responded to PEPPS while on failing therapies. Comparative Control. As an observational study, there were no control groups. To provide a comparative “control” experience, each veterinarian was asked to reflect on their respective experience and select from a choice of a clinical response times which they would deem to deviate significantly from the expectations of their clinical experience. Most of the small animal veterinarians (8.
This consensus of significant departure from expected time of clinical response was used to benchmark the primary outcome and a meaningful response. In essence, expectations of past clinical experience (replete with interventions requiring more time to work) served as a “comparative control” albeit a subjective one. Consent. All animals were privately owned and owners’ consent was obtained by veterinarians. Veterinarians Participating in the Study.
Veterinarians placing orders for commercially available PEPPS were recruited to participate in this open- labeled trial. Each had more than 5 years of professional practice. Veterinarians were recruited from June 2. December 2. 00. 6.
All veterinarians prescribing PEPPS were engaged exclusively in primary care of small companion animals. They were experienced in the standards of care in treating vomiting and diarrhea in dogs and cats. Out of 2. 56 small animal veterinarians, 1. Veterinarians received no honorarium for their participation. Sequential Participation. Participation in the study was sequential, determined solely by the order of spontaneous requests for product made by veterinarians responding to notification of product’s availability.
The veterinarians were self- selected. Information prompting orders pertain to the usefulness of PEPPS in the management of vomiting and diarrhea in small animals. Inclusion/Exclusion Criterion for Dogs and Cats. Dogs and cats were brought to the veterinarian by clients primarily due to vomiting and/or diarrhea. Included in the trial were dogs and cats with vomiting and/or diarrhea for more than 3 days with or without bleeding and dehydration. Animal’s symptoms were attributed to gastrointestinal infections from viral, bacterial and protozoan agents or to exposure to environmental toxins.
Notable inclusions were animals described by veterinarians as having hemorrhagic gastroenteritis, parvovirus enterocolitis, gastritis, intestinal “flare- ups”, and pancreatic “flare- ups”. Cases of food intolerance were included.
No cases of medication induced vomiting or diarrhea included. Excluded were animals requiring surgical intervention. Test Population. Animals included dogs and cats of varied age, breeds and weights. The size of the test population was 3. Vomiting- dominant and diarrhea- dominant was defined by the major concern of the client who initiated the visit. Also included were 2.
All patients were studied across multiple office- based practices. The population was also geographically diverse with input provided from 4. US. 3. 8. Conditions Managed. Inappetence, vomiting and diarrhea fail owners’ attempts to adjust the pets’ diet. Following evaluation by physical exam, lab tests and in some cases x- rays the clinical impressions of veterinarian covered a broad range of diagnoses that included hemorrhagic gastroenteritis, parvovirus enterocolitis, gastritis, reflux, suspected ulcer, intestinal “flare- ups”, pancreatic “flare- ups” and “stomach issues”. The severity of GI symptoms or the presence of other (non- surgical) disorders did not preclude patients’ involvement in the study.
Cases of food intolerance were included. There were no cases of medication induced vomiting or diarrhea in this study. Both dogs and cats were brought to the veterinarian due to vomiting and/or diarrhea. Existing Treatment Regimens in Dogs and Cats. Methods of management for small animals were diverse. Existing treatment regimens for dogs and cats prior to PEPPS varied widely and included antibiotics, anti- emetics, acid reducers, pancreatic enzyme supplementation, bismuth preparations, plain sucralfate and dietary changes. To these diverse regimens PEPPS was added.
Veterinarians in the study opted to add PEPPS to existing regimens that had been deemed inadequate or insufficient by them. There was no PEPPS only test group. Primary Outcome Measure in Dogs and Cats. There were two symptom- related primary outcome measures for this trial—the cessation of diarrhea and the cessation of vomiting.
The cessation of these symptoms within 2 days or 4 doses of PEPPS represented a positive outcome. This veterinarian- defined response to therapy was accepted as a meaningful clinical response (as described in section on Study Design) for the management of vomiting and diarrhea in dogs and cats in this study.
Clinical observations made by veterinarians were reported by phone for data collection.
How to Prevent Diverticulitis Naturallyistock. This is a guest post written by staff nutritionist Kelsey Marksteiner, RD. Click here to read her blog or join her newsletter!
If you’ve ever experienced a diverticulitis attack, I’m sure you’d be the first to say that it’s not a pleasant experience. I bet you’d be willing to do a lot of things to prevent it from happening again! Or maybe you’re someone who has been diagnosed with diverticulosis by your gastroenterologist, but you’re not quite sure what to do to prevent those painful attacks you’ve heard about and you want to learn more. Whatever brought you here, I’m happy to have you. Today I’ll be providing tips on how to prevent diverticulitis attacks naturally.
What is Diverticular Disease? Diverticular disease is the term used to encompass a spectrum of issues from diverticulosis (the presence of sac- like pouches called diverticula that protrude from the colonic wall) to diverticulitis (the inflammation of these pouches and the accompanying symptoms). Diverticular disease is common in the Western world, with the highest rates seen in the United States and Europe. Even in those countries the disease was almost unheard of in 1. However, if you have diverticulosis and want be sure to prevent any problems or you. However, these recommendations are based on inconclusive research and may not provide much benefit to you. In fact, few studies show any benefit to avoiding nuts and seeds and one study even showed that intake of nuts and popcorn was associated with a decreased risk of diverticulitis and diverticular bleeding.
In fact, of 9. 30 patients undergoing surgery for symptomatic uncomplicated diverticular disease (SUDD), approximately 7. This is also why chronic use of non- steroidal anti- inflammatory drugs (NSAIDs) such as ibuprofen have been shown to increase the risk of diverticular complications . It is clear that chronic inflammation is involved in the development of diverticular disease, and that those who wish to prevent attacks should take steps to reduce intestinal inflammation. Thankfully, one of the best ways to decrease intestinal inflammation is to eat a paleo diet!
By avoiding potentially irritating and inflammatory foods such as grains and omega- 6 fatty acids, we can reduce intestinal inflammation and encourage proper gut health. A paleo diet also positively influences gut bacteria, which in turn results in reduced inflammation as well. A paleo diet for diverticular disease should focus on gelatinous cuts of meat, bone broths, well- cooked vegetables, starchy tubers, and fermented foods. Reducing your stress level is also important for bringing down levels of intestinal inflammation, as stress has been shown to activate inflammation in the intestine. This means incorporating mind- body activities such as yoga, meditation, tai chi, etc on a regular basis. This one is important!
Another way to reduce intestinal inflammation is to supplement with soothing and healing demulcent herbs – deglycyrrhizinated licorice (DGL) has been shown to reduce mucosal damage and inflammation in rodents . Take chewable DGL tablets or mix a spoonful of slippery elm or marshmallow root powder in a small amount of water and drink 1- 3 times per day to help soothe and heal intestinal inflammation. Another healing substance for the gut – bone broth – should be liberally consumed for this purpose as well. Altered intestinal bacteria. Small intestinal bacterial overgrowth (SIBO) is common in diverticulitic patients.
As Chris has mentioned, Prescript Assist tends to be the probiotic of choice for those suffering from constipation so start with that if you tend to err on the side of decreased motility. Prebiotics are also very useful for correcting dysbiosis, and should be considered by those with diverticular disease. My go- to prebiotic is Pure Encapsulations fructo- oligosaccharide (FOS) powder, but others include GOS and even lactulose. Supplementation with 1.
FOS per day has been shown to increase counts of bifidobacteria. However, if you tolerate them well I think prebiotics can be a powerhouse when it comes to correcting imbalanced gut flora. Most importantly, it. This is similar to what is found in patients with constipation predominant IBS and in functional constipation.
In studies on animals with a lack of ICC networks, delayed or absent intestinal motility is noted. Given that our stool is mostly made up of dead bacteria, one can imagine that without proper amounts of good bacteria we. Prebiotics can be particularly useful for constipation given that they selectively increase good bacteria like bifidobacteria. Serotonin concentrations in those with colonic diverticulosis are significantly lower than normal controls and contribute to the type of bowel habit following a test meal. In addition, it is also likely that supplementation with 5- HTP (a precursor to serotonin) may alleviate constipation and increase motility since it will increase serotonin levels. Note: do not take 5- HTP without talking to your doctor first if you are on an SSRI medication.
Second, if you. In my experience working with those with constipation on a paleo diet, this is the single most effective diet- based recommendation I. Note: since SIBO is so common for those with diverticulosis, this step may need to wait until that has been treated, and may not be appropriate for some people.
Magnesium supplementation can also be very useful for people with constipation. Given that only about half of US adults consume the RDA for magnesium . This is due to the fact that not many foods naturally contain high amounts of magnesium, and even those that do have less due to the depletion of magnesium from our soil.
Check out this magnesium soil content map to see how your local area is doing (and think about where most of your food comes from – if you. I’ll leave you with a set of action steps so you remember exactly what to do to improve these underlying factors.
Action Steps to Prevent Diverticulitis Attacks: Eat a paleo diet! Reduce stress. Use demulcent herbs such as DGL, slippery elm, and marshmallow root to soothe and heal the intestine. Take probiotics like VSL #3 or Prescript Assist. Take prebiotics like FOS powder. Treat SIBO or dysbiosis. Reduce intestinal inflammation to increase SERT functioning, and consider supplementation with 5- HTPIf you? Chime in on the comments below!
This is a guest post written by Kelsey Marksteiner, RD. Kelsey is a Registered Dietitian with a Bachelors degree in nutrition from NYU, and is currently working on her Master’s in Human Nutrition and Functional Medicine. She works in private practice and recommends individualized dietary therapy focusing on biologically appropriate diet principles to aid her clients in losing weight, gaining energy, and pursuing continued health. She is a firm believer that everyone is different, and she tailors her plan for each and every individual. Through her work, she aims to meld the dietary wisdom of traditional cultures with the latest science in integrative and functional medicine to create plans for her clients that work in the modern world. You can learn more about Kelsey on her.
Join her newsletter here! Like what you’ve read? Sign up for FREE updates delivered to your inbox.
I hate spam too. Your email is safe with me.
 RSS Feed
RSS Feed
